Isabella Bizzotto is a 28-year old Italian nurse specialising in anesthesia and intensive care.
She’s been working at the University Hospital in Padua (which is in Veneto, one of the hardest hit regions in Italy) since the beginning of the COVID-19 outbreak.
We spoke to her about life on the front lines, the daily challenges she faces trying to protect patients and her wish for the Irish people.
Tell us about your job and how it’s changed?
So, when we started receiving COVID-19, my hospital had to create an extra Intensive Care Unit for those patients. Now we have 11 extra beds. After this, they split the intensive care staff into two, to cover both units. The operating room is closed at the moment, so their staff have come to support us.
Staff with families or older relatives at home are only working with ‘normal’ patients. This is to reduce their risk of exposure to the virus. I work with both infected and non-infected patients, but from next week this will change. I will only be taking care of COVID-19 patients from next week.
The situation sounds very stressful, how are you and your colleagues coping?
Yes, it is. We’re taking care of double the amount of patients, under incredibly difficult circumstances.
Yesterday two colleagues in another intensive care unit tested positive, but with no symptoms. That means we’re down two health workers in one day. If we get infected, we need to stay home and this is a huge problem. We don’t have enough staff to cope with this emergency already.
Have you been tested yet?
No, I haven’t because I do not have any symptoms and I haven’t been in direct contact with someone positive. Now, there are many doctors and nurses who have tested positive for COVID-19.
If you worked with them you are considered high risk, so they test you. All the staff are necessary at the moment, it is extremely important that we don’t get sick.
What special protective equipment do you need to stay safe?
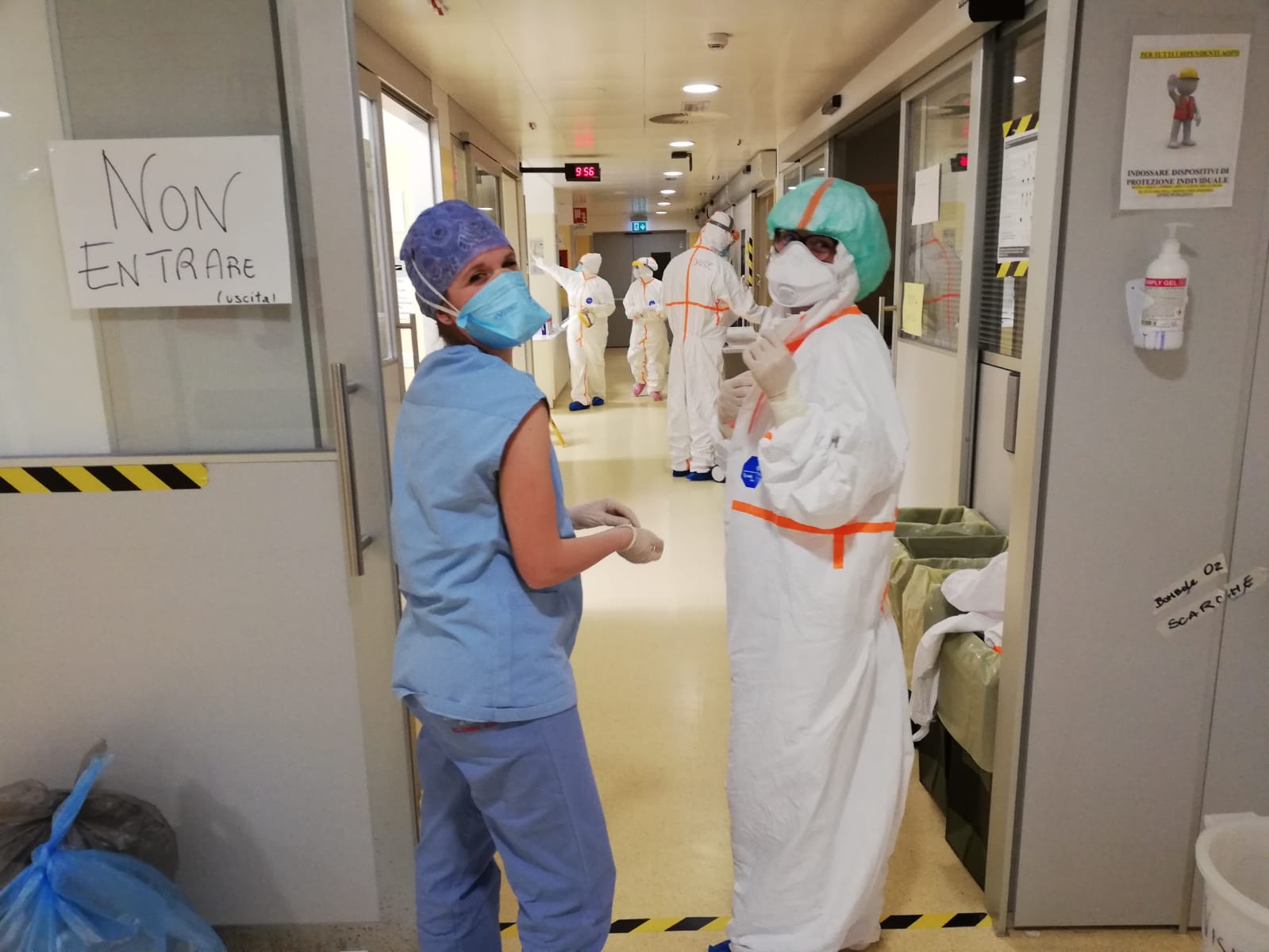
We absolutely need to have Personal Protective Equipment (PPE). The mask must have a FFP2 filter when you deal with infected patients. A normal surgical mask doesn’t protect you if the patients cough in front of you. Another important tool is goggles. Some of us wear face shields, but also gowns, gloves and shoe covers.
The problem is that when you take care of patients you move around a lot and need to be careful not to expose any part of your body, and this is difficult. We constantly have to turn patients, sometimes they are really heavy but the priority is to take care of them first.
After a while you don’t even notice you’re wearing the heavy protective equipment. It is very very very hot though. It’s like you are wrapped in cellophane.

Do You Have Enough Equipment?
We survive day by the day.
At the moment, gowns, surgical caps and shoe covers are in short supply. Every shift, you’re never sure what equipment you are going to have. It’s frustrating because we need to protect ourselves.
How does your work now compare to before?
Now it is difficult to protect all the patients. For example when we have a new patient, maybe he hasn’t been tested yet or he’s waiting for the result, we need to be able to isolate him immediately.
If we make a mistake and put an infected patient with non-infected patients, we’re putting all their lives at risk. The other challenge is that we don’t know how long it will last and what is coming. Before, we’d only treat patients who needed intensive care, now we get everything.
Recently, a pregnant patient gave birth in the Intensive Care Unit. Normally she would have been transferred to the maternity unit. Thankfully, both mother and baby are recovering well.

What does a typical day on the ward look like?
I enter the prep-room, where I get changed and put on my Personal Protective Equipment. Then I go to meet my colleagues for the handover and I’m assigned my patients for the day.
Usually I deal with the most complex cases, as I’m specialised in intensive care, while many other colleagues, who’ve come from other units to help us, are not.
Once I’ve started my shift, I begin by visiting and checking my patients. I constantly check their vital signs, check how they’re breathing and then I do everything that the patient can’t do.
Patients in intensive care have a lot of pressure sores because they can’t move. Imagine if you had to lie down on your face, completely still, for 11 hours? They develop a lot of wounds caused by the pressure and we need to take care, treat them and ensure they’re comfortable.
We need to turn our patients on their stomach every 12 hours. This is to relieve the pressure on their chest. We need 6 nurses to safely turn a patient of normal weight, but sometimes we need up to 8 nurses. After that, I’ll transfer any patient that is fit and well enough to leave the unit.
What is your biggest challenge?
The unknown. For sure it’s a difficult situation because we don’t know enough about this virus. We are dealing with something new and unknown.
The fear. I’m constantly thinking about how I can protect everyone around me. Everyone at home, my colleagues and my patients. We know we are more at risk than anybody else and I feel scared if, for example, I’m in the elevator with somebody. I don’t want to put anybody at risk.
Another challenge is to keep doing your job in a situation that is unmanageable, from a management’s point of view.
They are hiring new staff and transferring staff from other units to help us. However, these colleagues are not prepared to deal with such complex patients. You need months to learn the basics when it comes to working in an Intensive Care Unit, but they have hours.
Our job is to ensure the safety of the patients, so we need to keep an eye on everybody and also help each other, because the life of that patient is in your hands. This is very stressful from a psychological point of view. And we can’t take any holidays until June or even later.
How does it feel working on the front line during this emergency?
I feel good knowing I’m useful and that I can make a difference. I can really help. When I’m at the hospital, I know it’s going to be a long day, that it could go wrong and that I will be exhausted, but at the end I feel I’ve done something important.
This feeling has never been more important. Our community needs us. I know I need to bite the bullet and keep going. I need to be there.
What advice would you give to Irish people during this crisis?
Stay at home.
By doing this, you won’t expose people to infection and you’ll also help the health system. If you slow down the spread of the virus the health system can cope with the patients and their needs.
It is very difficult to stay at home, but it is something you have to do for your own community. The more people get the virus the more your community is at risk. We can’t expose people like those working in supermarkets or other essential services to the virus. They have the right to be safe, they are working because they have to.
Also we need to make people who are alone, feel we are there for them. I’m thinking also about people with the virus but without symptoms, they need to stay isolated at home. They are scared and afraid, they don’t know what will happen to them, how the disease will progress. If tomorrow they will be still able to breathe. The anxiety for these people is huge. You know you are sick but you don’t know what your future looks like. Nobody can go to your home to help you. You are alone.
We need to support the most vulnerable people and be there for people who have no one. Our sense of community needs to be stronger than ever.
If you’d like to support health workers like Isabella, please donate now to our COVID-19 appeal.

